Lipedema and lymphedema are both chronic conditions suffering from a lack of awareness and accessible treatment and this blog will highlight the similarities and differences in lipedema vs lymphedema.
I’ll discuss appearance, location, symptoms, diagnosis, treatment, and diet, plus I’ll link to lots of helpful resources
Appearance of Lipedema vs Lymphedema
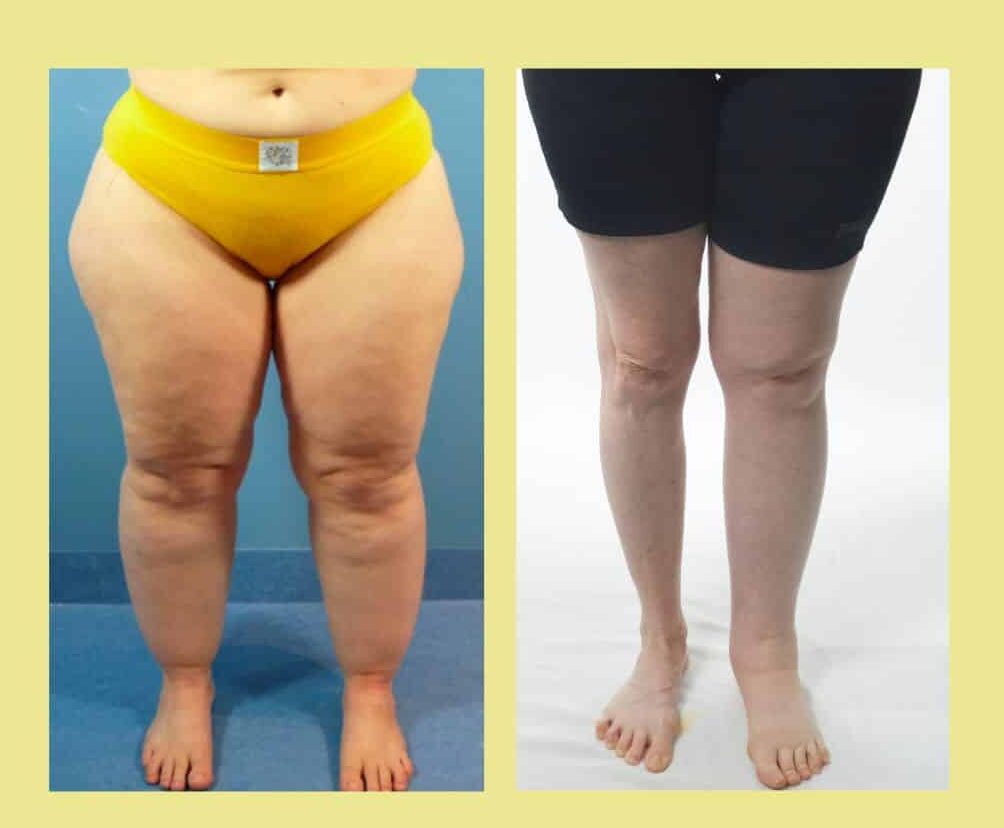
Both conditions result in a swollen appearance on the parts of the body affected, but there are ways to tell them apart.
While it can appear on all parts of the body, lipedema tends to occur more on the hips and thighs and can go as far as the ankles. It is next common on the arms, sometimes just the upper arm but can go all the way to the wrists. It’s important to note that lipedema occurs mostly in women while lymphedema can occur in men and women.
Lipedema can look like orange peel skin, or bumpy looking skin. For this reason it is often misdiagnosed as cellulite.

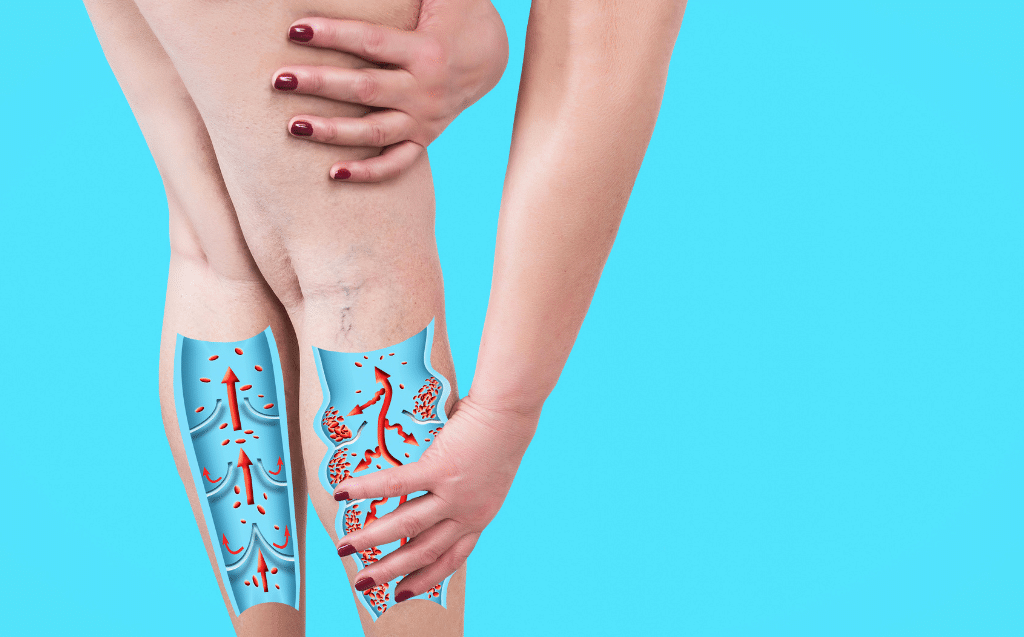
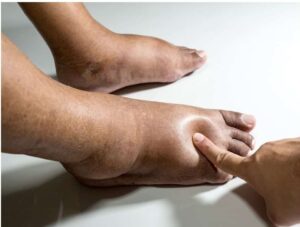
Lipedema tends not to affect the hands or the feet, while lymphedema can cause swelling all the way to the toes and fingers. Lymphedema also has pitting edema present in the early stages.
It’s important to note that some people have both conditions and this is called lipo-lymphedema. This means they will have symptoms from both conditions.
Location of Lipedema vs Lymphedema
Lymphedema has two main types: primary and secondary. While there is no standard presentation, primary tends to be either throughout the body or in one or sometimes both legs. But, lymphedema is often worse on one side than the other.
Secondary lymphedema will occur in a localized area depending on the injury to the lymphatic system. For example if a woman has lymph nodes removed from her left arm pit as part of breast cancer surgery, her lymphedema will occur on the left arm, breast or chest wall. It’s common for lymphedema to occur only in one arm, one leg or one breast.

Lipedema on the other hand, tends to be more symmetrical from right to left. The distinguishing feature of lipedema is that it is disproportionate from upper body to lower body. For example, someone with lipedema may wear a size 8 on the top and a size 12 on the bottom.

Symptoms of Lipedema vs Lymphedema
The symptoms of lipedema include pain, fatty nodules under the skin, easy bruising, and inability to lose lipedema fat. Eventually joint problems can develop, usually in the lower back, knees and ankles due to the presence of large bulges of fatty nodular tissue.
Lipedema pain varies and can be minimal to intense. Women have described being unable to hold a cat or a baby on their lap due to the pain. Unlike most people who find massage to be relaxing, a woman with lipedema can find massage to be too painful and intolerable.

The symptoms of lymphedema include aches, pain, heaviness of the affected area, reduced joint range of motion and swelling. Individuals with lymphedema are also susceptible to cellulitis – a skin infection that requires immediate medical attention for antibiotics.
In some cases, lymph fluid can leak through the skin – called lymphorrhea, this is appears as clear liquid on the skin surface. If not taken care of with compression and wicking bandages, a wound can develop.
Diagnosing Lipedema vs Lymphedema
Unfortunately, both lymphedema and lipedema are chronic and progressive and getting an early diagnosis and treatment is critical. Getting a diagnosis for either condition can be challenging as there isn’t a lot of awareness or a medical speciality for either. While it’s more common for an oncologist or rehab medicine specialist to see lymphedema, likely the most trained in recognizing it would be a vascular (vein) specialist.
The specialists that may be most familiar with lipedema would likely include specialized plastic surgeons, bariatric physicians or a connective tissues disorders physicians. If you are having difficulty finding a physician to diagnose you, then seek out a certified lymphedema therapist in your area, and they can likely recommend a knowledgable physician.
Diagnosing lymphedema would begin with a medical history. It’s important to provide information on past injuries, surgery or cancer treatment. If there is not history of any of this, then you may more likely have primary lymphedema, in which case, a family history will be important, as primary lymphedema is a genetic condition and knowing if your parents or grandparents had swollen limbs will be helpful.
There are several genetic markers that have been identified for lipedema and lymphedema. It’s recommended that children with primary lymphedema be tested. This way, if the gene can be identified it will help the family to prepare for what’s to come – either with progression of lymphedema or other known co-morbidities.
Some genetic lymphedema’s don’t progress much and have no other co-morbidities, but some do, and identifying the type will help to plan the best treatment and further testing (Gordon, 2020).
Lymphoscintigraphy is a sophisticated test used to help diagnose lymphedema. A radioactive tracer is injected into the skin between the toes or fingers and imaging is used to visualize how well the lymphatic function. Unfortunately, this test is not available at all hospitals, but thankfully, it is not required for diagnosis.
A physical exam would include a check for a stemmer sign. This is a very low tech, but highly accurate diagnostic tool (Goss, 2019). You can do this by pinching the skin between the toes (or fingers if your hand is affected) to see if the skin will tent. Skin that does not tent, is a “positive stemmer sign” and is diagnostic for lymphedema.

Diagnosing lipedema would require a physical exam – mostly manual exam to find fatty nodules, easy bruising, looking for tell tale joint issues, like hyperlordodic spine, screening for common concurring conditions like Ehlers Danlos syndrome or eating disorder. A family history is also important. While genetic tests are available for lipedema, there are more genetic markers to be discovered, so a negative genetic screen would not rule out lipedema (Michelini, 2022).
Treating Lipedema vs Lymphedema
There are similarities in the conservative treatment for these two conditions, the gold standard of treatment is called complete decongestive therapy and it consists of compression, skin care, exercise and manual lymphatic drainage.
The first step after your diagnosis should be to find a certified lymphedema therapist. To find one in your area, see my blog on lymphedema resources that has links to organizations and training programs that provide databases that you can search by location to find a therapist near you.
In addition to these, there are many complementary therapies for lymphedema that show benefit. Some of those complementary therapies include low level laser, reflexology lymphatic drainage and scar therapy.
Additional therapies for lipedema include myofascial release, compression pumps and deep breathing. But, the main treatment for lipedema is specialized liposuction such as tumescent liposuction, water-jet assisted liposuction (WAL) or laser-assisted liposuction. Read more about these in my blog Lipedema Treatment.
Diet for Lipedema vs Lymphedema
There are many similarities in diet recommendations for both lipedema and lymphedema. Since both conditions are inflammatory, an anti-inflammatory approach makes good sense for both. Drinking plenty of water, and minimizing salt, can help prevent fluid retention and allow fluid to be moved from the swollen areas.
An elimination protocol can also be helpful for identifying food triggers and/or determining if there is a gastro intestinal connection with symptoms.A ketogenic approach has been recommended for both, but there is more research to support the use of keto for lipedema than keto for lymphedema.
But keto is definitely not the only option and the diet plan should be tailored to the individual. To read more details check out lipedema diet and lymphedema diet.
Recommended Reading
If you have lymphedema or lipedema, it’s important to educate yourself about your condition. Unfortunately, you can not rely on your medical doctor as these conditions despite affecting millions of people are not part of most health care curriculums. In addition to the links above, check on these related blogs:
References for Lipedema vs Lymphedema
Ghods M, Georgiou I, Schmidt J, Kruppa P. Disease progression and comorbidities in lipedema patients: A 10-year retrospective analysis. Dermatol Ther. 2020 Nov;33(6):e14534. doi: 10.1111/dth.14534. Epub 2020 Nov 22. PMID: 33184945.
Gordon K, Varney R, Keeley V, Riches K, Jeffery S, Van Zanten M, Mortimer P, Ostergaard P, Mansour S. Update and audit of the St George’s classification algorithm of primary lymphatic anomalies: a clinical and molecular approach to diagnosis. J Med Genet. 2020 Oct;57(10):653-659. doi: 10.1136/jmedgenet-2019-106084. Epub 2020 May 14. PMID: 32409509; PMCID: PMC7525776.
Goss JA, Greene AK. Sensitivity and Specificity of the Stemmer Sign for Lymphedema: A Clinical Lymphoscintigraphic Study. Plast Reconstr Surg Glob Open. 2019 Jun 25;7(6):e2295. doi: 10.1097/GOX.0000000000002295. PMID: 31624689; PMCID: PMC6635205.
LaMantia, J DiMenna A. The Complete Lymphedema Management and Nutrition Guide. Robert Rose, 2018.
Michelini S, Herbst KL, Precone V, Manara E, Marceddu G, Dautaj A, Maltese PE, Paolacci S, Ceccarini MR, Beccari T, Sorrentino E, Aquilanti B, Velluti V, Matera G, Gagliardi L, Miggiano GAD, Bertelli M. A Multi-Gene Panel to Identify Lipedema-Predisposing Genetic Variants by a Next-Generation Sequencing Strategy. J Pers Med. 2022 Feb 11;12(2):268. doi: 10.3390/jpm12020268. PMID: 35207755; PMCID: PMC8877075.